It’s Still Safe to Visit the ER
Across the country, ER waiting rooms are significantly less busy than usual.
“Emergency care physicians across America are asking, ‘Where are all the heart attack and stroke patients?’,” said David Lang, D.O., medical director of emergency medicine at the University of Miami Health System.
“We don’t want patients sitting at home with worsening conditions. In most emergency cases—especially in cases of stroke and heart attacks—timely treatment dramatically improves patient outcomes and saves lives.”
Critical care providers like Dr. Lang are urging the public to seek immediate medical attention when needed. “Waiting gives us less opportunity to prevent worsening symptoms,” he says.
Call 911 or go immediately to an ER if you or a loved one is experiencing:
- chest pain
- difficulty speaking
- mental confusion
- difficultly moving an arm or leg
Seek immediate medical attention if a child is:
- displaying sudden changes in behavior
- having an asthma attack
- has a high fever
If you’re concerned but aren’t sure a situation requires an ER visit, call your primary care physician, or use the telehealth system to ask a medical professional for guidance.
“We are very well prepared to see and treat people with all kinds of medical emergency needs—not just those with COVID-19 symptoms and infections,” Dr. Lang says.
Across the U.S., hospital emergency departments and urgent care facilities are following enhanced protocols for managing cases of COVID-19 while protecting other patients and healthcare workers. These efforts include disinfecting surfaces, ventilating airspaces, and wearing effective protective gear (PPE).
Patients are being screened and triaged upon arrival.
“If we suspect a patient has or possibly has COVID-19, we treat them in a separate area of the E.R.,” Dr. Lang says. “Patients who are determined to have a low suspicion of COVID-19 infection are sent to a different area of the E.R.”
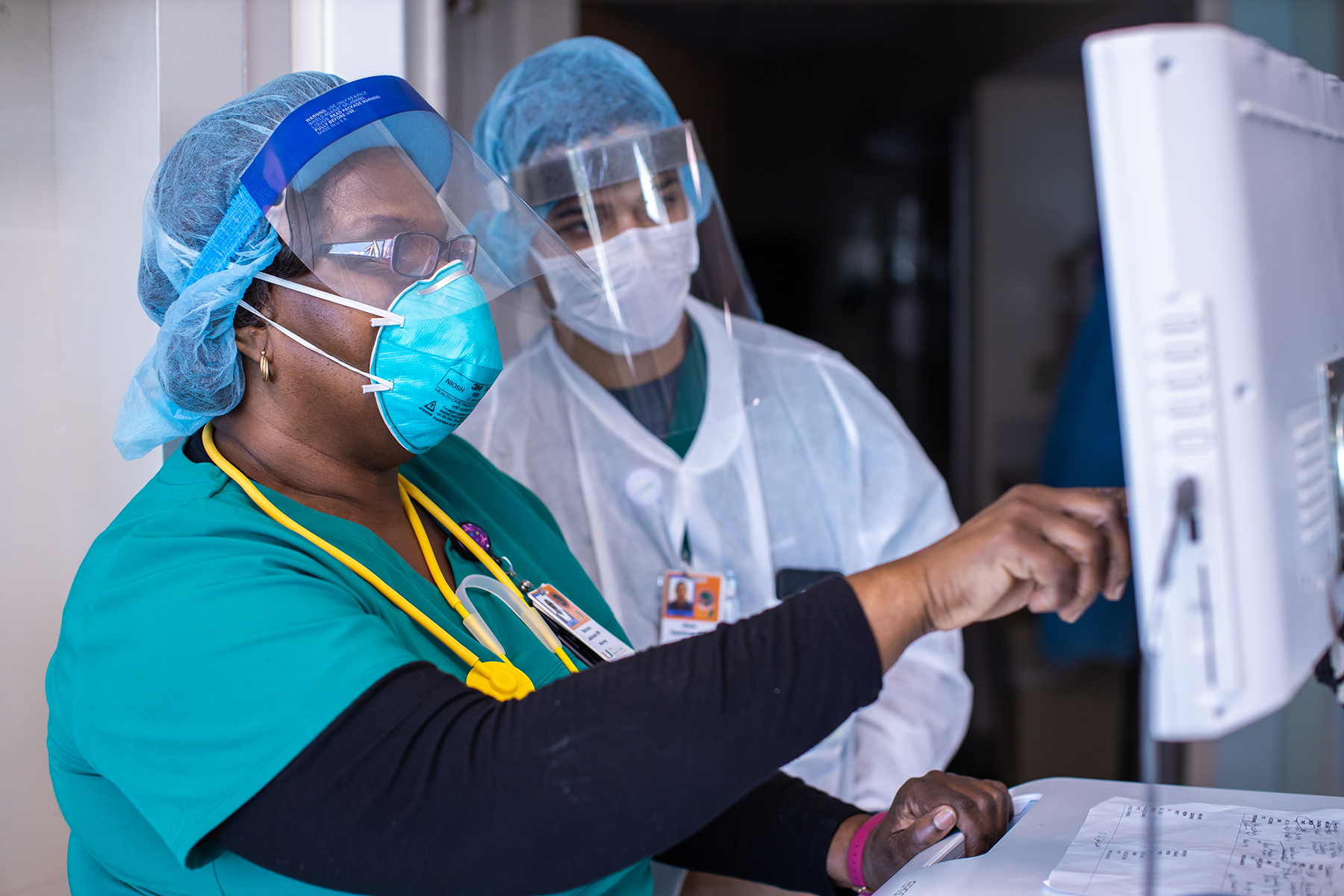
At UHealth, staff wear masks, gowns, gloves, and face shields. Masks are supplied to incoming patients.
ER nurses are assigned to certain zones. So, those caring for COVID-19 patients do not also handle non-COVID-19 patients. “The last thing we want to do is bring a contagious virus from one patient to the next,” Dr. Lang said.
“Wherever you are, don’t delay essential medical care out of fear.”
Dana Kantrowitz is a contributing writer for UMiami Health News.
