Can Artificial Intelligence Improve Your Next Mammogram?
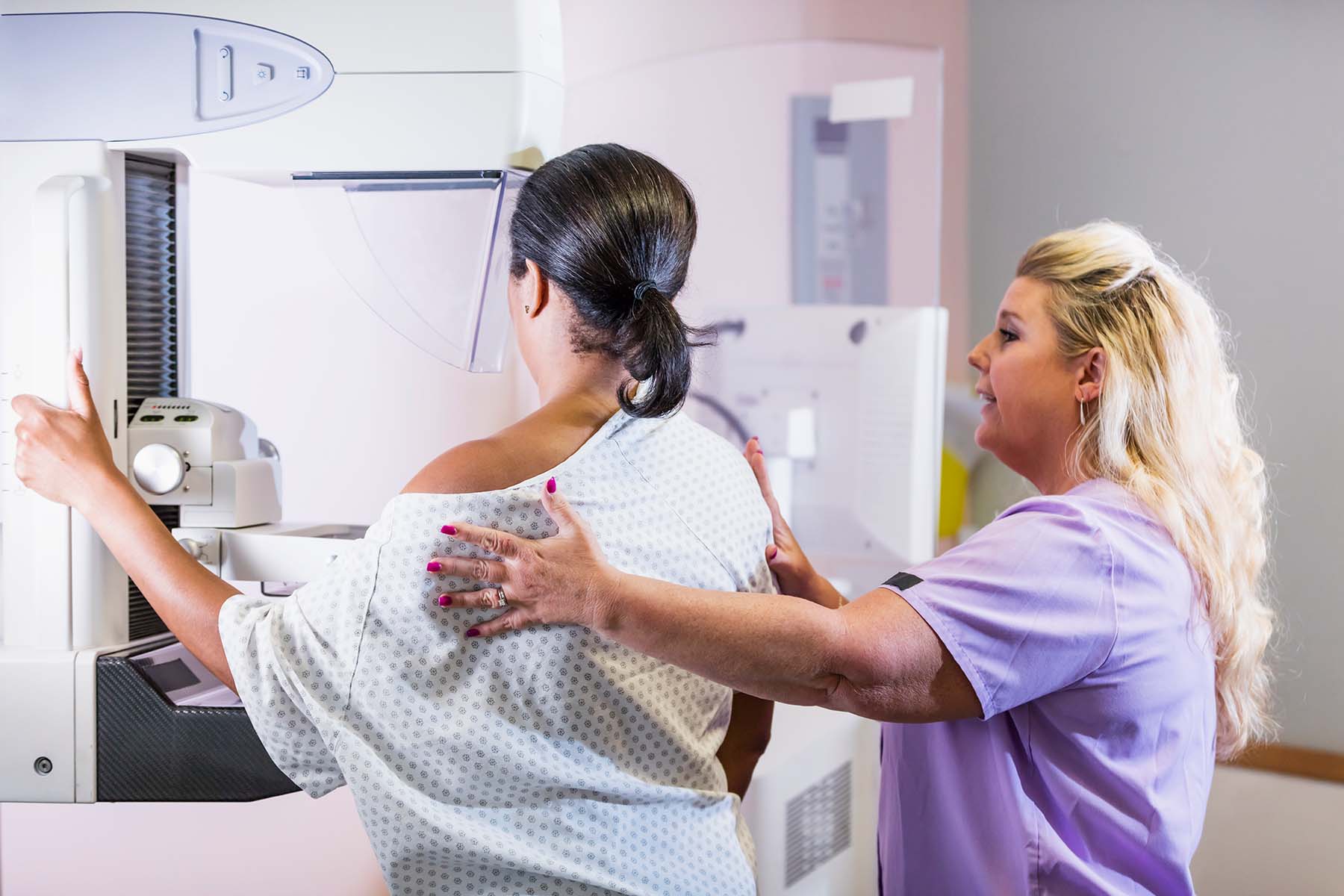
Radiologists tap technology to improve accuracy, reduce false positives, and the need for repeat mammograms.
Artificial intelligence once seemed like science fiction, but it is now woven into the fabric of our daily lives. Just ask Alexa.
Health care is no exception. About seven years ago, radiologist Fernando Collado-Mesa, M.D., F.S.B.I., was surprised to hear information technology experts predict that “AI” would replace radiologists like him and put them of work.
Radiologists are medical doctors who interpret medical imaging exams (X-rays, CT scans, MRI, etc.).
They also perform image-guided procedures to diagnose and help treat diseases and injuries.
Not one to ignore technological advances, Dr. Collado-Mesa researched AI in earnest. Today, he’s confident AI will not replace radiologists who spend about 13 years learning their craft. Instead, it will assist them and make them more effective and efficient.
For patients getting mammograms, that means the potential for greater accuracy and a better chance of detecting breast cancer early, when it’s most treatable. Up to 13% of cancers are missed when a mammogram is read, according to one study. AI could also help reduce false positives – about 10% of patients must return for additional testing, a costly and stressful experience.
Humans are irreplaceable
As director of Innovation and Artificial Intelligence at the University of Miami Miller School of Medicine’s department of radiology, Dr. Collado-Mesa uses his knowledge to improve patient care at Sylvester Comprehensive Cancer Center, part the University of Miami Health System, and at Jackson Memorial Hospital’s Breast Health Center, where he is a medical director.
“Currently, mammograms at our facilities are read by expert radiologists assisted by an expert artificial intelligence program. This helps radiologists assess the density of the breast, a recognized breast cancer risk factor that can also ‘mask’ small breast cancers. In this human-machine relationship, the human component is irreplaceable.”
Like the AI model used at UHealth, other AI models for mammography have also received FDA clearance. Some are being considered for incorporation into the UHealth radiologists’ workflow. Combined, radiologists and AI are faster and more accurate at reading mammograms. Unlike humans, a computer never gets tired or distracted.
On the other hand, radiologists can integrate relevant patient information — including risk factors such as family history — with the findings on breast images and can then provide a more holistic approach.
Personalizing AI to our community
Developing AI for clinical use is a cross-disciplinary effort. Dr. Collado-Mesa collaborates with the University’s Electrical and Computer Engineering Department and the Institute for Data Science and Computing.
“We are training AI models to perform as well as a human expert at tasks such as predicting patients’ response to breast cancer therapies.”
AI has advanced tremendously, but there is still a lot of work to be done, including work to prevent bias.
“We must expose these types of medical AI programs to images of patients from different ethnicities,” Dr. Collado-Mesa says.
For example, if UHealth purchased an AI software developed and tested on images from ethnic groups different from those in our community, it might not perform as well as reported by the AI model vendors.
“We are going to help develop and test AI tools tailored to the population we serve in our community. We can also test an AI product (developed elsewhere) and train it for our population.”
To help fine-tune the technology, the AI team is building a massive database of anonymous clinical data and medical images. In addition to the imaging data, it includes risk factors such as race and ethnicity, socioeconomic and educational status, and exposure.
“This has the potential to transform local radiology,” Dr. Collado-Mesa says. Having a tool that draws data from millions of South Florida patients while maintaining their privacy will help UHealth radiologists be more comprehensive and precise. The hope is that this will guide doctors to perform early diagnosis and determine the most effective treatment for specific demographic groups of people.
One technology, many uses
Particularly exciting is AI’s potential to address several health issues in a single imaging exam.
“We can train the model to look at multiple anatomic structures,” says Dr. Collado-Mesa.
“For example, studies show an association between calcifications present in breast arteries and cardiovascular disease. Heart disease, not breast cancer, is the number one killer of women. In the future, a mammogram could reveal your risk of cardiovascular disease. From one exam, we could get more comprehensive health information, adding value to a routine annual screening you already do, at no additional cost or radiation.”
Eventually, AI systems will touch every aspect of the medical imaging cycle.
They will assist with appointment reminders, schedule appointments, search patient medical records, and flag pertinent information for the doctor’s use. AI will also help with the actual acquisition of the images and improve their quality.
With AI, images will be presented to the radiologists to help them detect and diagnose breast cancer and help with follow-up recommendations and management.
“If there are things such as a family history of breast cancer that the doctor should be aware of, the system will bring that to the doctor’s attention,” Dr. Collado-Mesa says.
In his role as assistant director of the University’s Diagnostic Radiology Residency Program, Dr. Collado-Mesa is training the next generation of doctors to use this technology.
“Radiology residents and fellows are being taught about AI through lectures, and interested trainees participate in AI research.”
Transformation doesn’t happen overnight.
“We have to be methodical. We are working with Sylvester Comprehensive Cancer Center and our Institutional Review Board to test a commercially available AI product in our population that helps radiologists detect cancer on breast MRIs,” Dr. Collado-Mesa says.
As sophisticated as AI has become, “Humans will always be involved.” Integrating AI into health care is a painstaking process but has far-reaching benefits for patients and doctors. By improving efficiency and accuracy, the technology will allow radiologists to spend more time with patients, be more personalized in their approach to treatment, and double down on their efforts to save lives.
Nancy Moreland is a regular contributor to UMiami Health News. She has written for several major health care systems and the CDC. Her writing also appears in the Chicago Tribune and U.S. News & World Report.
Tags: diagnose, health disparities, imaging, radiology, targeted diagnostics, technology in medicine
