CRISPR: A New Frontier in Cancer Research
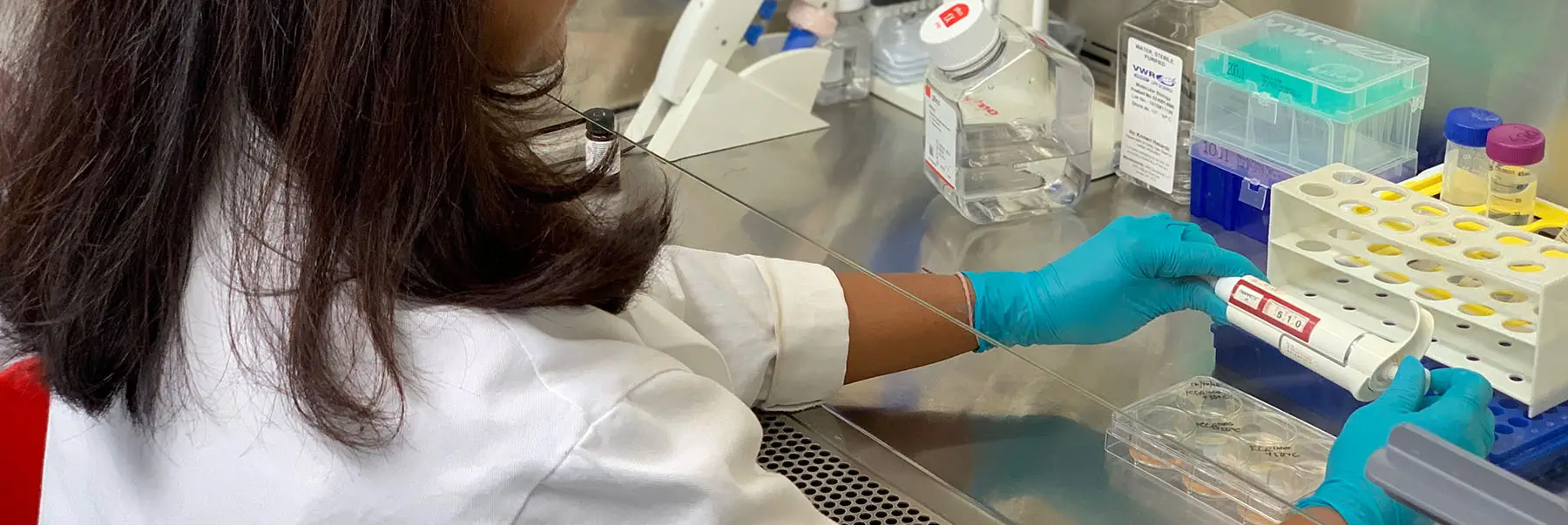
Imagine a group of scientists using blood stem cells to create a malignant tumor in mice, a tumor that one day might help them and other researchers experiment with potential cures for a scourge that can now only be treated with chemotherapy.
It may sound like science fiction — but it isn’t. In a lab at Sylvester Comprehensive Cancer Center, Dr. Jonathan Schatz and his team of scientists have used CRISPR, the genomic editing tool, to force specific chromosomal changes in blood stem cells that are then transplanted into mice. These transplanted cells eventually cause lymphoma tumors in these mice.
That is a simplified explanation for a complex process that Dr. Schatz’s team has pioneered. The Sylvester researchers have come up with a new way to develop a mouse model of a blood malignancy by using the much-touted CRISPR. Other researchers, he explains, have used the genomic editing tool to cut problematic DNA information and then replace it with a snippet of different genetic material. Dr. Schatz, however, has created a change in the genetic material that eventually results in a cancer.
What is CRISPR?
CRISPR – known as CRISPR-Cas9 in scientific circles —is short for clusters of regularly interspaced short palindromic repeats. It’s originally a defense mechanism in certain kinds of bacteria, but it’s been engineered to work like molecular scissors. That’s because Cas9, an enzyme, can cut strands of DNA.
Certain characteristics of CRISPR allow scientists to cut and correct DNA sequences to modify gene functions. “In a research setting the potential applications are unlimited,” explains Dr. Schatz, an associate professor at the medical school. “CRISPR is an extremely powerful tool because it allows for genomes to be edited in a very precise and effective way.”
Since its development a few years ago, CRISPR has become a powerful research tool in the laboratory.
It’s also been used to improve crops and has a wide variety of potential medical uses, especially for genetic diseases, but most of these are at early development stages. Perhaps the most attention-grabbing use of CRISPR was revealed in November 2018 when a Chinese scientist claimed he had used CRISPR to edit human genes in order to make a pair of twin girls resistant to HIV, an announcement that shocked the science world as most researchers agree this new tool is not ready to be used on humans.
In Dr. Schatz’s lab, researchers did not correct or prevent the expression of a disease. Instead researchers were able to create in mouse blood stem cells the same rearrangement of chromosomes found in a human cancer. They created a system that instructs the Cas9 protein to cut at two particular parts of the DNA. When those breaks in the middle of the DNA happens, they sometimes form a translocation of the genes — think of it as genes switching partners. These cells with the translocation are then transplanted into mice to replace the animal’s own blood stem cells that have been radiated out of existence.
Fast forward more than nine months and these translocated cells begin to develop as anaplastic large cell lymphoma, a cancer of the lymphatic system that is usually found only in adolescents and young adults.
In the pilot experiment, three out of the four mice developed this cancer “which was very similar to the lymphoma in humans.” The fourth mice developed a different, and rarer, kind of lymphoma, also found in humans. Currently Dr. Schatz’s team is waiting on a new batch of mice that have been transplanted with these translocated genes. “We’re about five or six months away from seeing results,” he explains.
Other researchers, he points out, have transplanted “aggressive combinations of cancer-causing genes” to speed the development of cancer in lab mice for studies. But he prefers “a natural progression of the disease that mimics the human progression more closely. Instead of forcing it, we wanted only the chromosomal translocation.”
Now, the Schatz team is using CRISPR to create oncogenes — genes with the potential to cause cancer — that will develop into other lymphomas and leukemias.
“By creating models of a disease in the lab it gives us a system to study the biology of the disease,” Dr. Schatz explains. “It will also enable us and other researchers to do treatment experiments to develop and optimize therapies.”
The team’s findings were presented at the annual meeting of the American Society of Hematology in December 2018. The study is now in peer-review for publication.

Ana Veciana-Suarez, Guest Columnist
Ana is a regular contributor to the University of Miami Health System. She is a renowned journalist and author, who has worked at The Miami Herald, The Miami News, and The Palm Beach Post. Visit her website at anavecianasuarez.com or follow @AnaVeciana on Twitter.
Tags: Ana Veciana Suarez, blood stem cells, CRISPR, Dr. Jonathan Schatz, genomic editing, Sylvester Comprehensive Cancer Center
