Does Cupping Help Ease Stomach Issues?
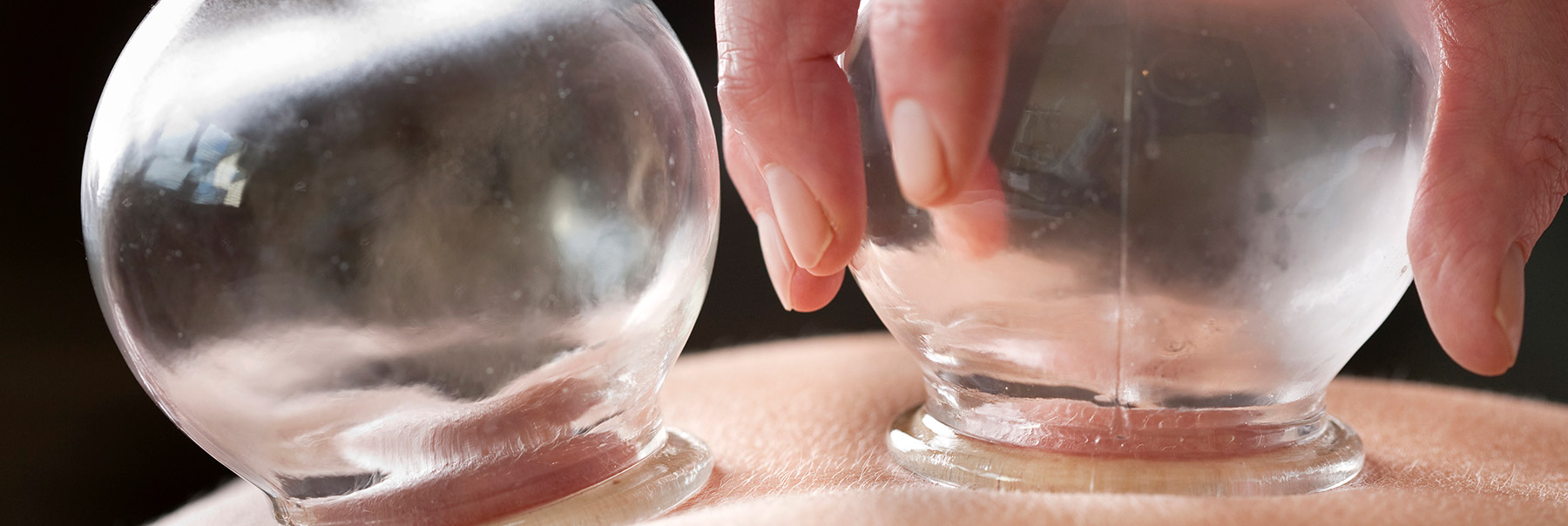
The ancient therapeutic practice of cupping can allegedly relieve a variety of ailments. Practitioners and devotees say it helps with issues ranging from arthritis pain and widespread inflammation to chronic hives and psoriasis. But when it comes to digestion, the science isn’t there, experts say.
What is cupping?
There are two main types of cupping: “wet,” which involves puncturing the skin (called bloodletting), and “dry,” which doesn’t. Both techniques use glass or ceramic cups, alcohol, and a flame to vacuum-seal the cups to the skin for about 10 to 15 minutes. This is most commonly done on the back and is recognizable from the red or pinkish circular marks it leaves behind on the skin for a few days.
Can cupping improve your gut health?
Some holistic wellness clinics promote dry cupping on the abdomen to ease GI distress. Providers may claim this technique can help clear colon blockages, stimulate digestive organs, promote bowel regularity, eliminate toxins from the body, help bolster and regulate gut health, improve digestion, and soothe abdominal pain.
But “I was unable to find data on cupping and GI diseases—likely because no randomized controlled trials have been done,” says Michelle Pearlman, M.D., a board-certified gastroenterologist with the University of Miami Health System. “I do not recommend cupping to treat GI distress.”
Even without the support of certified specialists, those suffering from gastrointestinal symptoms, including upper abdominal pain, bloating, diarrhea, and constipation, might turn to complementary and alternative medicines in search of relief. “Patients with food sensitivities, intolerances, or food allergies might try cupping when it’s difficult to identify the triggers causing GI discomfort,” Dr. Pearlman says.
Because cupping isn’t proven effective in treating these GI conditions, Dr. Pearlman recommends a more reliable approach.
“One of the best ways to try to identify potential food sensitivities, allergies, and/or intolerances is to use a food diary and take notes on your symptoms and when they pop up,” she says. “Discuss these findings with a registered dietitian or healthcare provider to identify potential food triggers that may be contributing to your GI distress. Your food diary may also reveal nutritional deficits you can discuss with your doctor, as well.”
Dana Kantrowitz is a contributing writer for UMiami Health News.
Tags: cupping, Dr. Michelle Pearlman, gastrointestinal health
