Eczema: How to Manage the Itch-Scratch Cycle
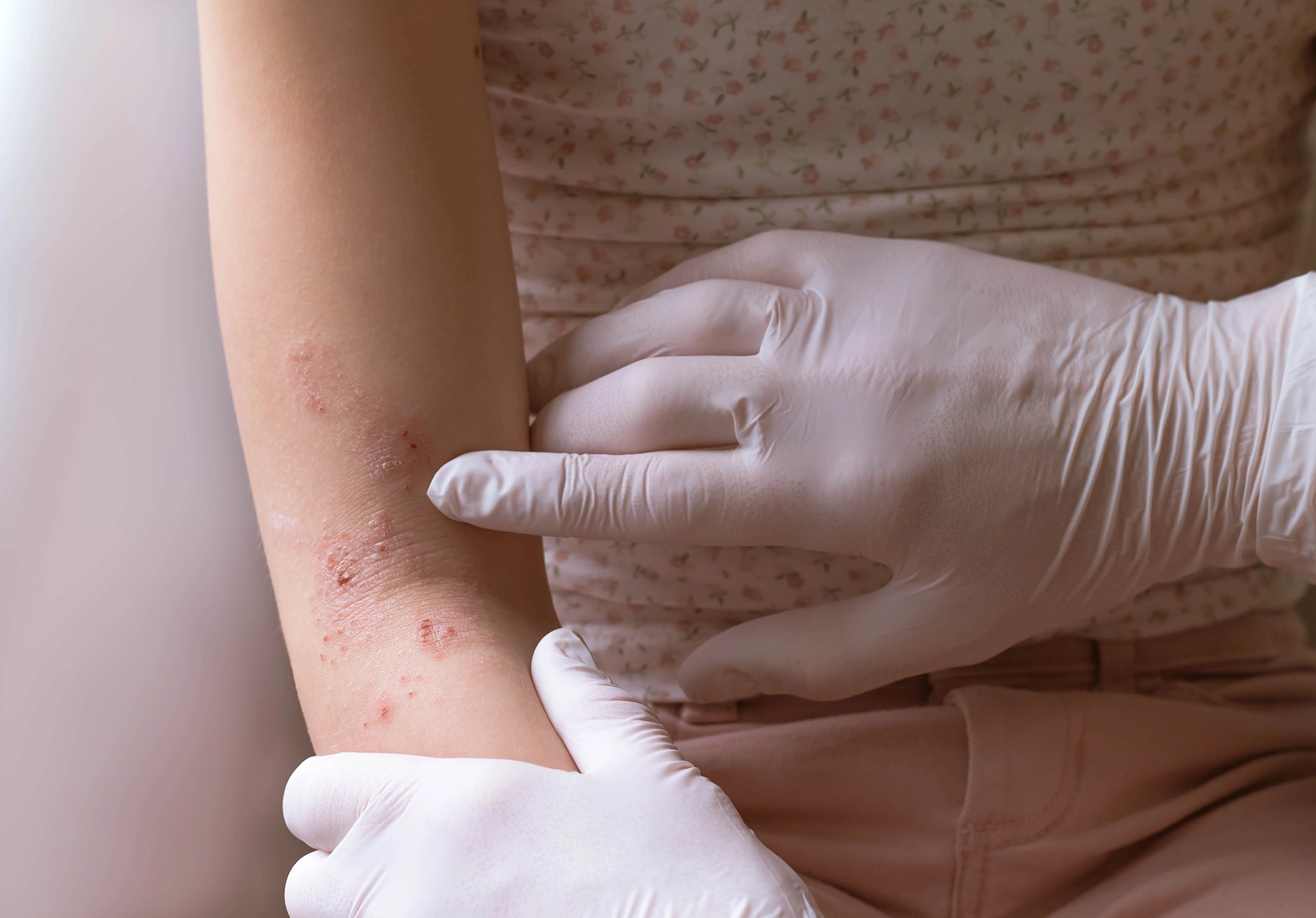
Eczema isn’t a single dermatological disorder. Instead, it’s a group of related skin conditions with one irritating thing in common: itchiness.
Other symptoms like red, scaly, inflamed skin are also common with eczema. Scratching at these flare-ups can feel unavoidable at times, but doing so can break this delicate skin and cause bleeding, infection and worsening irritation while prolonging the healing process. If you scratch enough, the skin and nerve damage can intensify all of these symptoms and trigger another skin condition called neurodermatitis. So, what can you do to help clear up an eczema flare-up and prevent it from recurring?
Is that rash actually eczema?
Eczema typically shows its ugly head during childhood and sticks around for years or becomes a chronic, lifelong condition. For some, it develops during adulthood.
It can look and feel a lot like many other skin conditions. So, it’s best to have your skin examined by a dermatologist to get an accurate diagnosis. In addition to a physical exam, your doctor may conduct a blood test, patch test and/or biopsy to confirm the diagnosis and cause of your eczema and determine the best way to treat it.
Eczema flare-ups tend to have poorly defined areas of redness with dry, fine scales. This scaling can appear silvery, white or red. In adults, eczema patches may get thicker, rougher, darker and leathery in texture. In children especially, eczema can develop in the skin’s creases and folds, like the hands, feet, ankles, wrists, neck, upper chest, eyelids, elbows and knees (in infants, on the face and scalp). Adults are more likely to see eczema patches on the face or hands.
Eczema can come and go, and the severity of it can vary.
Additional symptoms include:
- red to brownish-gray patches
- small, raised bumps that can leak fluid and crust over when scratched
- cracked skin
- raw, sensitive, swollen skin from scratching
- burning pain sensation
What causes eczema?
Eczema is an overactive immune response triggered by environmental factors and/or stress (physical or emotional). This condition can run in families, so it has a genetic component. Sometimes, it’s accompanied by asthma or hay fever.
Eczema flare-ups can be caused by:
- emotional stress
- extremely cold/hot or dry/humid weather
- contact with allergens (like grass, pollen, pet dander, mold, dust mites and insect bites)
- ingestion of food allergens
- stress or injury to the body (such as surgery, illness or accident)
- exposure to irritants (like certain chemicals, materials, metals and ingredients in household, skin and beauty products)
When you see the National Eczema Association Seal of Acceptance on any product, you can rest assured that it’s free from known eczema irritants.
How can I manage eczema flare-ups?
Skin Care
- Use only gentle, fragrance-free products designed for sensitive skin (including mild cleansers).
- Clean and gently dry the affected areas daily.
- Keep the affected areas hydrated/moisturized.
- Avoid picking, scratching, and rubbing the affected areas as much as possible.
- When spending time in a dry, cold or hot environment, protect your skin with clothing and a product like petroleum jelly, which provides a hydrating barrier.
Self-care
- Because emotional and physical stress can trigger or worsen eczema flare-ups, lowering your stress level can reduce flare-ups and lessen their severity and length. Ways to reduce stress on the body include getting enough sleep and exercise, and practicing mindfulness/meditation.
- Eat an anti-inflammatory diet, like the Mediterranean diet, which limits alcohol, added sugars and processed and fried foods.
- While more research is needed to confirm their effectiveness, some people with eczema experience symptom relief with wet wrap therapy, acupuncture and cryotherapy.
- Avoid any known eczema triggers to reduce the frequency and severity of your flare-ups.
Ointments and Creams
- Apply an over-the-counter, fragrance-free, sensitive skin moisturizer to keep the upper layers of your skin protected and hydrated.
- Some moisturizers include cooling agents and anti-itch ingredients like oatmeal or pramoxine.
- Apply an over-the-counter or prescription-strength steroidal ointment, cream or lotion to reduce inflammation and itchiness. Use these products as directed, as topical corticosteroids will thin and weaken the skin when applied regularly or for long periods.
Oral and Injectable Medications
- New prescription drugs called targeted oral small molecules and injectable biologics are extremely effective at interrupting inflammation, controlling eczema and enabling some people with this disease to achieve full remission.
- Discuss with your doctor the risks associated with taking a biologic.
It can take time and trial and error to figure out which products or environmental factors contribute to your eczema breakouts. Your dermatologist may have additional recommendations for your daily skincare, relieving eczema flare-ups and preventing future symptom breakouts.
Dana Kantrowitz is a contributing writer for UHealth’s news service. Medically reviewed by Gil Yosipovitch, M.D., dermatologist with the University of Miami Health System.
Tags: chronic itch, Dr. Gil Yosipovitch, flaky skin, skin care in Miami
