Mantle Cell Lymphoma – A Personal Journey

As an oncology dietitian, I have had the honor of supporting cancer patients for more than 30 years. But, it wasn’t until I became a patient myself that I truly understood how essential it is to have a strong support system.
It all started last June. The first thing I noticed was that I had lost nine pounds after my annual physical when everyone else was gaining weight because of the pandemic. Then, I noticed that suddenly my legs felt like lead when I climbed the stairs to my bedroom or tried to run after work. And I had a lot of heartburn. But, I explained away my symptoms until my family urged me to go back to the doctor.
When my lab work came back, my doctor called me and said, “You need to see a hematologist. Your blood work is all over the place.” However, I needed to get a bone marrow biopsy before I could see a specialist.
When I walked into the clinic, I was scared to death.
I’ve been on the other side of the door when I’ve heard people getting it, and it’s not pleasant.
Thankfully, though, a nurse practitioner who I’ve known since I started working at the university was there to perform the procedure. She hugged me and said, “I promise you, I’m going to be as gentle as I can.”
She blasted one of my favorite musicians, Michael Bolton during the procedure. She talked me through the procedure and kept me very calm. I was shocked that it was not nearly as horrible as I had anticipated.
I had my diagnosis 72 hours later — mantle cell lymphoma.
I don’t know what I was thinking. I just was in shock.
The weird thing is, as a clinician, I’ve always gravitated towards pancreatic or head and neck cancer patients. I felt like I made a difference with them because they had a lot of GI issues, and I could help them.
Although I volunteered for the Leukemia & Lymphoma Society for years, running marathons or doing lectures and presentations, I generally didn’t have patients with that type of cancer. And, now I was one of them.
Go to a NCI-designated center.
I am grateful that I worked at Sylvester Comprehensive Cancer Center. I knew a National Cancer Institute-designated facility offers many more opportunities than just going to your community hospital. But, having experienced it cemented that for me, there are so many choices out there that I have now. Also, my doctors and the whole clinical staff became family to me.
I chose Alvaro Jose Alencar,M.D., as my medical oncologist. Although, I really didn’t know him. I knew his wife, a nurse practitioner, and I had worked with her previously.
During my first visit, I said, “I’ve got two grandchildren I need to see grow up.” He said, “Oh, you will.”
He said that if I had been diagnosed 10 years ago, I probably wouldn’t have many options. But, in the last three to five years, there’s been a lot of research on mantle cell lymphoma. He assured me that there were now lots of options out there.
My treatment plan included six cycles of chemotherapy and immunotherapy – three outpatient and three in the hospital – followed by chemotherapy and a stem cell transplant.
After three treatment cycles, I had a PET scan for restaging and met with Dr. Alencar. He asked me how I felt, and I said, “Honestly, I kind of feel like I did before I got diagnosed.”
He said, “Well, you should ’cause you’re in remission.”
I was on cloud nine, but I knew there was still a lot ahead of me.
The week before my first hospitalization, they told me I couldn’t get treatment there because the COVID-19 transmission rates were too high. I was concerned that I would not be treated; instead, I just had another outpatient treatment.
I finally did get the two treatments in the hospital. After that, they did another PET scan and bone marrow biopsy, and I was still in remission. So, it was time to turn me over to the transplant team, headed by Dr. Beitinjaneh. They started collecting my cells so I could have a stem cell transplant.
Suddenly, though, it seemed like everything was going super-fast. It was freaking me out. I had to get a port placed in my chest. It was three tubes dangling from my chest.
It was extremely uncomfortable trying to take showers, but it made it so much easier in the long run when they had to give me chemo, blood transfusions, and hydration. They collected my cells over two days. It reminded me of donating platelets, where they take the blood out of you, put it through a centrifuge, and then put it back in.
My hospital stay was three weeks.
For the first six days, I had to get chemotherapy with four different drugs. The one on the last day was the one I was dreading because it was one that they said I could probably get mouth sores with it.
They said, “You’re going to chew ice 30 minutes before we start. Then, you’re going to chew ice the whole time we’re giving it to you, and then you’re going to chew ice for another hour after you’re done. That’s going to reduce the risk of you getting mouth sores.”
I did not want a mouth sore, so I chewed, and I chewed. And then they came in and said they were waiting on pharmacy. And then they returned and said, “It’s gonna be a little while. You can stop chewing.” And I thought, heck no, and I continued to chew.
Five days later, I started feeling like there was this tiny sore on the left side of my tongue that hurt when I talked. I could eat on the other side of my mouth; it was more annoying than anything. I don’t think it even lasted a week; I was lucky.
The transplant was like a Sci-Fi movie.
They came in with a container, and when they opened it up, all of the steam came out. I had one nurse hanging the cells and getting them through the port to be delivered to me. Then I had these two people that were over by this container.
There were eight bags of my cells; they would take one bag out and put it in a hot water bath to thaw it. And then the nurse would take it and put it through the port. The whole process was less than an hour.
After the procedure, I sat in the hospital for two weeks, watching paint dry. My blood counts were wiped out, and now we were waiting for everything to start working again.
But now, I was beginning to get nausea from the chemo, and I would wake up every morning and feel … ugh. I would throw up just once, but it was just enough to make my whole day feel yucky. They finally figured out the right anti-nausea drug combination, which wasn’t so bad.
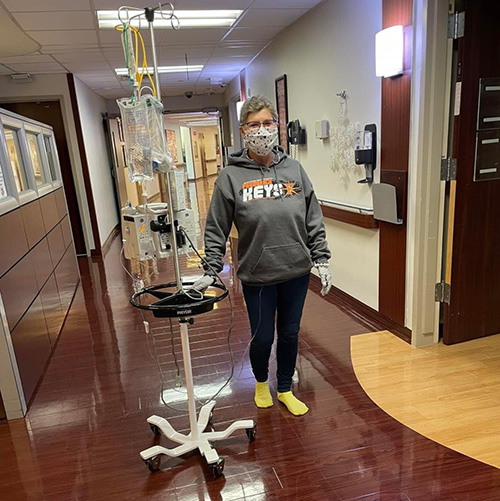
I made sure that every day I got up, took a shower, ate what I could, and walked 15 minutes, three times a day in the hall. If I was attached to the IV pole because I was getting hydration, I schlepped that pole with me.
Many people had their doors open, and I would see people lying in bed. I’m thinking, “Get out of the bed; you’re never going to get out of here if you’re not moving.”
Plan ahead and be proactive
I knew that the chemo was going to cause diarrhea. I recommend to a lot of my patients with diarrhea a product called Enterade. It helps with hydration and healing the villi in the small intestine to increase surface area for better absorption, so you don’t have as much malabsorption.
So, I started drinking it before I was admitted to the hospital, and then I ordered it in the hospital. But, after a week, I couldn’t get it down anymore. I still felt like I was getting some benefit from it, even though I had to stop drinking it.
Also, I brought a container of Banatrol with me, which is really banana flakes. It’s a water-soluble fiber, so if I had a bout of diarrhea, I would order some oatmeal and sprinkle it in there and get it in that way.
I was at the hospital over Passover. I brought two boxes of matzo with me. We know that when Moses said, ‘Let my people go,’ it was really about constipation because matzo will do that to you. So, I thought it would help me, and if I’m nauseous, it’s just a dry cracker. I’ve read charts where patients had terrible diarrhea. I had nothing like that. It was very manageable.
I tried to think far in advance about what I could do to help myself.
I even scheduled patients for follow-ups eight weeks out. I said, “You’re my incentive to come back to work because I think I should be ready by such and such a date.” So I tried to plan ahead and be positive about everything.
I got out of the hospital two days early.
I’ve had a couple of patients who have told me that they’re going into the hospital and will be there for several days. I’m trying to plan for them, helping them understand what they need to do to take charge.
I’ve been exceptionally fortunate support-wise.

My work family has been nothing short of amazing. My friends and family stay with me. They’ve helped me get through this whole thing. I don’t think I could have done it by myself.
You have no idea how good it feels to not worry about work and income while going through such a catastrophic event.
The day I got my first chemo, I posted about it on FaceBook, saying, “I’m not looking for sympathy. I’m looking for cheerleaders because I’ll have some tough days, and I need people to keep me positive.” And that’s exactly what they did. People came out of the woodwork, even friends I made in elementary school. It’s been amazing.
Regarding losing your hair. Well, it is what it is.
Laughing a lot helps. You can call me GI Jane, and I won’t slap you; I promise you.
I’ve really surprised myself. I know I can be fairly vain and that my hair has always defined me. Losing it was one of the hardest things.
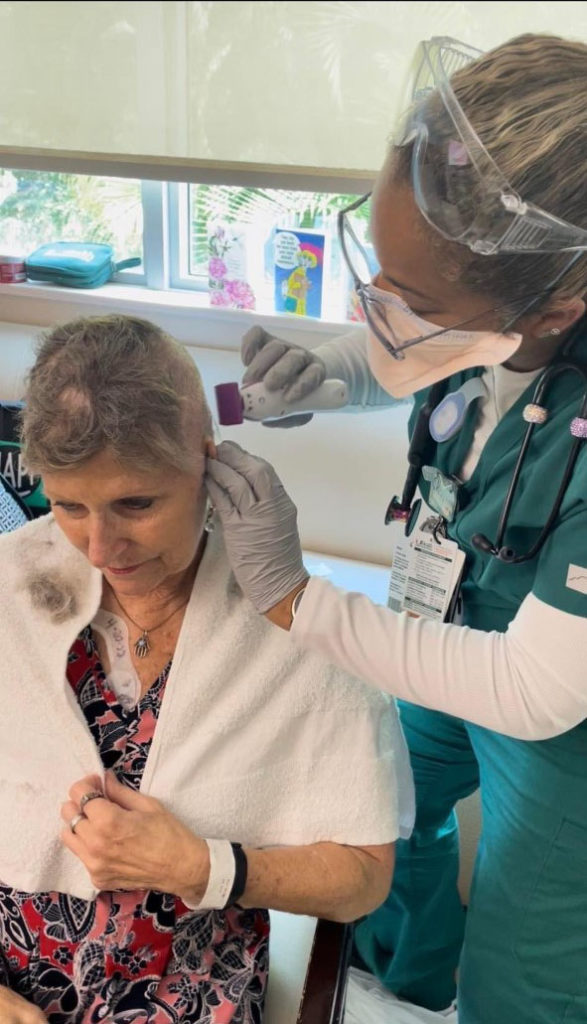
I already had it cut very short before I went to the hospital. But while there, I woke up, and my hair fell out in clumps. The nurse came in, and I looked at her, and I said, “This looks ridiculous; what am I gonna do?” She had clippers.
I thought it would be easy because my hair was so short, but it was pretty emotional.
The nurse was amazing. She talked me through it and put on music. We were both singing, “Mama said we’d have days like this.” The patient experience person who was coming in daily videoed the whole thing for me while she was shaving my head. It was amazing. I would never wish this on my worst enemy, but it wasn’t as horrible as I expected.
I have embraced a lot of scarves and hats. I’ve only worn a wig twice. Sometimes I’ll walk outside to throw something in the garbage and realize I didn’t put anything on my head. And it’s like, “I don’t care.”
Yeah, the head is what it is. My hair is starting to grow back – it’s tiny fuzzies right now.
Fight cancer with your fork – that has always been my stance.
I am an oncology dietitian, after all. But the food was just awful, and I am not picky. I found myself sitting around in my hospital room, thinking I’ve always been a patient advocate, but I need to do more. I kept thinking, “I feel okay, but what about the people that don’t feel good? How are they going to get better if they’re not eating?”
With my patients, I would go over the “textbook” eating healthy.
- Make sure you get good sources of protein.
- Eat lots of fruits and veggies.
I know sometimes you’re not going to feel great, but these are the things you should be doing. But, when I started having issues with changes in taste during my six months’ worth of treatment, everything tasted too sweet. It was gross.
One night my boyfriend said to order the Chicken Francaise, thinking the lemon sauce may make it not taste as sweet. I said, “No because chicken tastes horrible, and I don’t usually eat batter-dipped foods. I don’t eat stuff like that.” But I went ahead and ordered it.
It was one of the best meals I’ve had in a long time.
Then it clicked.
I had a handout called FASS for Troubled Tastebuds; fat, acid, sugar, salt.
Four things that can make food taste different.
If you’re having a change in taste, those foods can help, but I never actually applied it. I would give it to patients and tell them to try it; now, I recognize how it worked. An orange is easier to eat because even though it’s sweet, it’s still more acidic. On the other hand, the melon was sickeningly sweet.
The other thing was, especially in the hospital, my blood pressure was very low due to the chemo. So, I needed sodium. Also, I went back to when I was pregnant many years ago. Salt always helped settle my stomach when I had morning sickness.
I found that the hospital’s menu did not necessarily have a lot of sodium, because people don’t think of sodium as being healthy.
So, I asked my friends to bring me egg drop soup, my comfort food. It’s got protein because of the eggs and the sodium, so it will make my stomach feel better. Also, somebody brought me all-beef hot dogs. The sodium settled my stomach, and I knew I was getting some protein. Is it the best choice? Absolutely not. But it got me through so that I had the energy to get out and do my exercise every day.
It’s a marathon. Go the distance.

On this journey, I’ve just focused on little bits and pieces along the way – trying not to look at the whole picture all the time. It’s the same way I run marathons. I don’t stand at the starting line of a marathon and say, “I have 26.2 miles ahead of me.” I say, “I get to run for four minutes and then I have a one-minute walk break.”
I know what the end goal is, but I need little pieces to get me there.
I probably have three years of maintenance coming up, and I know there’s not a cure for me right now, but I’m in remission. The purpose of the stem cell transplant was to keep me in remission for as long as possible. So, if I can be in remission for 20 years, that gets me into my 80s, and then we’ll talk about the next step.
But if I can’t stay in remission that long, I know there are other things I can do because there’s been so much research.
I’ve done fundraising for Leukemia and Lymphoma Society over the years. My very first marathon I ran with them, I did in honor of one of my patients who passed when he was 28 years old. I continued running and coaching all these years in his memory.
While he was my patient, I always thought I was trying to save his life. Now, I feel like maybe he was trying to save mine. Down the road, I’m benefitting from all of that fundraising that has led to the research.
Now, 17 people, plus all my kids, are training for the Marine Corps Marathon on October 30th. It’s my all-time favorite marathon, and I’ve done it five times.
This time, they’re running it in my honor and raising money for more research. They’re paying it forward for someone who hasn’t already started their cancer journey. Their name is Team Go the Distance because of Michael Bolton. During my initial biopsy, ‘Go the Distance’ came on, and that’s my motto.
I am going the distance.

Lesley Klein, M.S., RD, LD/N is a registered dietitian and clinical oncology dietitian at Sylvester Comprehensive Cancer Center.
Tags: cancer care in Miami, Lesley Klein
