Pancreatic Cancer: What Should You Know
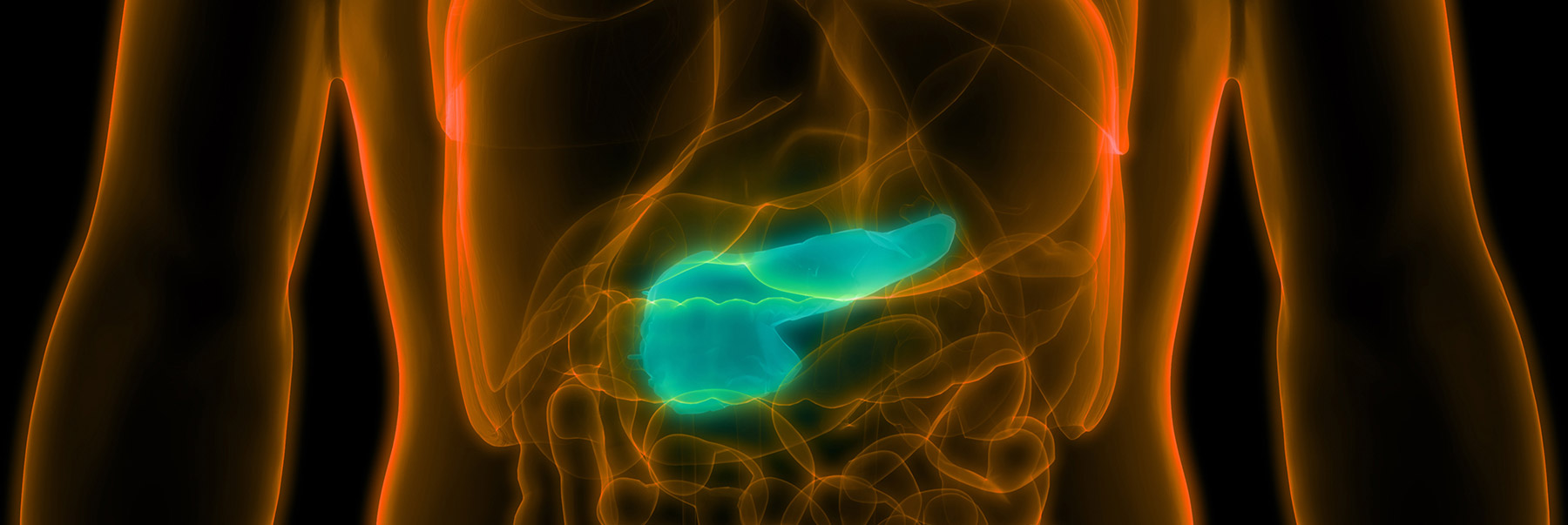
Rates of pancreatic cancer are rising.
When people list their specific cancer fears, most think of lung, skin, and breast cancers.
According to the American Cancer Society (ACS), pancreatic cancer makes up about 3% of all cancer cases in the United States or about 60,430 new cases in 2021 – but account for about 7% of cancer deaths.
“Deaths from forms of cancer like lung cancer and breast cancer have been decreasing in many western countries,” says Peter Joel Hosein, M.D., a gastrointestinal cancer specialist at Sylvester Comprehensive Cancer Center. “But pancreatic cancer is the third leading cause of cancer death and is increasing in incidence.”
What is pancreatic cancer?
When someone has irregular cells in their pancreas that grow and divide out of control, a tumor, which could be benign or malignant, may develop.
The pancreas is a gland that produces hormones to control your blood sugar levels and enzymes to help with digestion.
The most common form of a malignant tumor is called pancreatic ductal adenocarcinoma. It begins in cells that produce digestive juices, called exocrine.
The ACS estimates that the five-year survival rate for all stages of pancreatic cancer at 10%. Localized forms of the cancer are at 39%. When it has spread to other parts of the body, the rate is approximately 3%.
Stay aware of the risks
One aspect that makes pancreatic cancer so problematic, says Dr. Hosein, is that there have been no reliable screening tools. “If a person is at high risk of pancreatic cancer due to a strong family history of the disease or genetic risk factors, we will recommend annual MRI exams or endoscopic ultrasounds to check for signs of cancer,” he says. “But there aren’t many screening tools beyond that for an average-risk person.”
During 2021, one potentially significant advancement has been a “blood biopsy” test that works by looking for fragments of DNA in a person’s blood. This test can detect the presence of more than 50 types of cancer. “It’s not covered by insurance, but could be a way individuals at high risk can get screened for pancreatic cancer, among other cancers,” says Dr. Hosein.
Even still, Dr. Hosein says that the best way to manage the risks is to control the factors you can. “The rising rates of cancer may be related to living a sedentary lifestyle, rising obesity rates, and smoking,” he says. “So, you can protect yourself by maintaining a healthy weight, quitting smoking, and making other healthy lifestyle choices.”
At the United European Gastroenterology virtual meeting in October 2020, researchers presented a study that looked at 20 years of data from 1.4 million people. They noted a significant decrease in the risk of pancreatic cancer among the more than 10,000 people in the study who had weight-loss surgery.
How can I tell if I have pancreatic cancer?
Most people with pancreatic cancer rarely exhibit any early symptoms.
If you do notice these symptoms, it’s worth a visit to the doctor’s office.
- unexplained weight loss
- abdominal pain
- nausea, jaundice
- loss of appetite
- changes in your stools
The hurdle is that many doctors tend to identify these warning signs as something other than pancreatic cancer, says Dr. Hosein. “The Pancreatic Action Network has been encouraging patients to be vigilant about their health as a result of this. It’s important for patients to stick with it, get a second opinion if needed, and get to the bottom of their problems if they continue to experience these symptoms with no relief.”
Is pancreatic cancer treatable?
As with most forms of cancer, outcomes are better when it’s detected and treated early.
Chemotherapy is still the primary treatment method for pancreatic cancer, but immunotherapy appears to benefit some sub-groups, says Dr. Hosein. Research is continuing in this potentially promising area of pancreatic cancer treatment.
Patients at dedicated cancer centers, like Sylvester, tend to have better outcomes than those treated in other medical facilities. These patients have access to cutting-edge clinical trials that may make a tremendous difference for some patients. “For the early stages of the disease, it’s critical for patients to have a strong multidisciplinary team that consists of pancreatic surgeons, oncologists, radiation oncologists, dietitians, psychologists, gastroenterologists, interventional radiologists and more,” he says.
“You’re more likely to receive this level of care at a dedicated cancer center, as well as receive the most advanced treatment options.”
Wyatt Myers is a contributing writer for UMiami Health News.
Originally published on: November 09, 2020
