Unsightly Toes? You’re Not Alone
South Florida’s warm weather means that, for most of us, sandal season runs year round. We bare our feet with sliders, flip-flops slingbacks, and wedge footwear as much for comfort as to show off our (usually) manicured piggies.
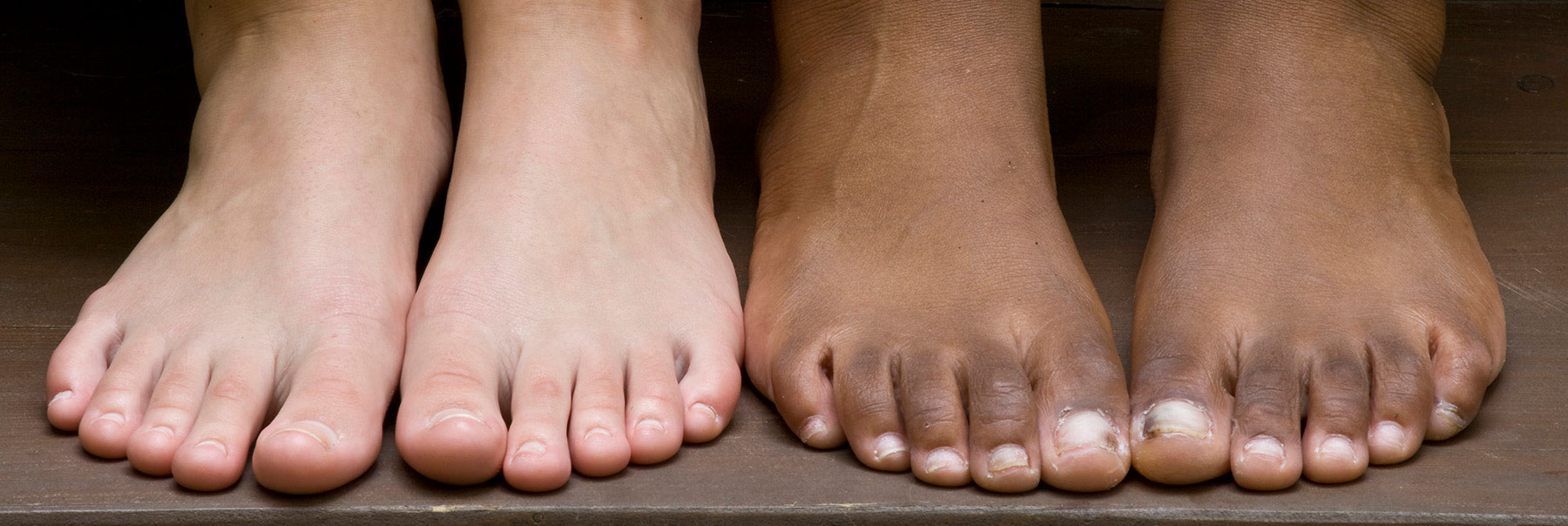
But what happens when feet aren’t worth exhibiting in public? When fungus turns a toe nail an unsightly yellow? Or thick callused skin roughens a heel? Or athlete’s foot causes scaly cracked skin between toes? The unsightly results of fungal infections to the feet are many — and unfortunately common.
“We do see quite a few people who come in for treatment,” says Dr. Andrea Maderal, dermatologist with the University of Miami Health System. “It’s mainly for toenail fungus because for most other conditions, such as athlete’s foot, people try to treat themselves with over the counter medications.”
The prevalence of these conditions is surprisingly high. As many as 50% of us will suffer from the toenail fungus, Dr. Maderal says, with the highest rate affecting people over 70. Athlete’s foot is even more common, as are tough-as-leather heels that remind us of elephant skin. Blame the hot, humid weather for athlete’s foot and toenail rot, both of which may start unobtrusively and then colonize our skin and nail bed before we have the sense to treat it.
What happens when fungi get a foothold
While none of these conditions are life-threatening, they can cause other problems. In some cases, people may suffer from pain or discomfort and, depending on the severity, even report having difficulty walking. A few may run the risk of medical complications, including cellulitis and bacterial infections.
For most of us, however, these foot afflictions are simply ugly and embarrassing — but not necessarily conditions one should ignore, to be sure. A 2014 study published in BioPsychoSocial Medicine found that those who suffer from toenail fungus and other nail dystrophies are often shunned for the disfigurement, leading to problems in their personal and professional lives.
What’s more, a condition like athlete’s foot can spread easily to other parts of the body. “Men can get it in their groin area [jock itch] from the fungus on their feet,” Dr. Maderal says. “It can be as simple as their underwear touching the affected areas and then moving up.”
Easy to get, hard to get rid of
Let’s start with the all-too-familiar athlete’s foot, also known as tinea pedis. It may be the most common skin fungal condition NOT seen by doctors, namely because most people treat it with an over-the-counter anti-fungal cream. Symptoms include scaling and itching of the feet, even blistering, usually between the toes. The condition is frustratingly easy to develop. Fungi thrive in locker rooms, swimming pool areas, gyms, communal showers, even at nail salons.
By walking barefoot in these areas, the fungi can be easily picked up.
What’s more, some people are genetically predisposed to get it, while others appear resistant to it. But because it’s so contagious, it can spread to other parts of the body, including your toenails, hands and groin area.
In fact, athlete’s foot can (and often does) develop into nail fungus, which is many times more common in toenails than in fingernails because our feet live in the hot and humid conditions that are ideal for fungi. “Many times it starts as athlete’s foot,” Dr. Maderal says. “It takes longer with the nail and it can be very subtle on the onset, but once it’s in the nail bed, it’s very difficult to get rid of.”
The first sign of a nail fungal infection is a white or yellow spot under the nail. The fungi then grows quickly on the nail bed, usually causing the nail to thicken and discolor. The overwhelming majority of cases, about 90 percent, are caused by a fungus called dermatophyte, while yeast and molds can be blamed for the rest of the cases.
Risk factors for nail fungus includes age, diabetes, HIV infection, immune-suppressed conditions and peripheral artery disease. If you are obese and smoke, your chances also increase.
Toenail fungus can be treated orally, usually over a three-month period. It should always be done under the close supervision of a physician, as prescribed medication can affect liver function and therefore patients must be monitored regularly during treatment. Dr. Maderal says the oral anti-fungal is about 80 percent effective, but even when the stubborn fungi is gone, she recommends patients be on the lookout for its return.
Re-infection is very common and not necessarily in the same nail. It has a way of moving on to other nails.
Dr. Maderal
While toenail fungus can be diagnosed by sight, doctors also like to “confirm presence of fungus by either microscopic examination of skin scrapings or by a demonstration of a fungus on a nail clippings,” Maderal adds.
Your brittle toes may not be the only unattractive foot problem to keep you away from those new sequined sandals.
Rough, thickened skin around the heel and sometimes on the sole can prove to be an all-too common eyesore. Known by its medical name, hyperkeratosis, calloused skin can also result in bothersome corns. In most cases, the skin is treated by humidifying lotions and protective padding over the offending areas. Dr. Maderal also recommends comfortable, well-fitting shoes.
The condition sometimes becomes painful or inflamed enough to send a patient to a doctor. These cases can be treated with a topical urea-containing lotion that softens the hard part of the skin, which in turn helps the dead skin cells slough off while keeping the new skin supple. In extreme cases of reddened or pus-filled areas, the skin should be immediately evaluated by a physician.
Non-fungal rashes can also wreak havoc on the appearance of our feet. Some causes include psoriasis, yeast and bacterial infections, eczema, even allergic reactions to creams or shoes. Toenails may be damaged by ill-fitting shoes, even by the way you walk. It’s best to visit a dermatologist for a precise diagnosis and proper treatment.
How to prevent the fungus among us
- Keep your feet dry. If your socks or shoes are damp, immediately take them off to dry.
- If your feet sweat a lot, use powder. Or try sweat-absorbing socks — or simply change them throughout the day.
- Dry, dry, dry and then dry your feet and toes some more after a shower or any time they’re wet. Don’t share towels or linens.
- Wear open-toed shoes as often as you can.
- Always wear flip-flops in public pool and gym areas.
- Treat your shoes with an anti-fungal powder (or disinfectant) — or throw them away — after an infection.
- Make sure your nail salon uses sterilized tools after each customer. Disinfect your own nail clippers after each use.
- Choose comfortable shoes that give your toes space to breathe.

Ana Veciana-Suarez, Guest Contributor
Ana is a regular contributor to the University of Miami Health System. She is a renowned journalist and author, who has worked at The Miami Herald, The Miami News and The Palm Beach Post. Visit her website at anavecianasuarez.com or follow @AnaVeciana on Twitter.
Tags: Ana Veciana Suarez, dermatology, Dr. Andrea Maderal, fungus, toenail
