COVID-19 Vaccines are Safe for Pregnant Women and Teens
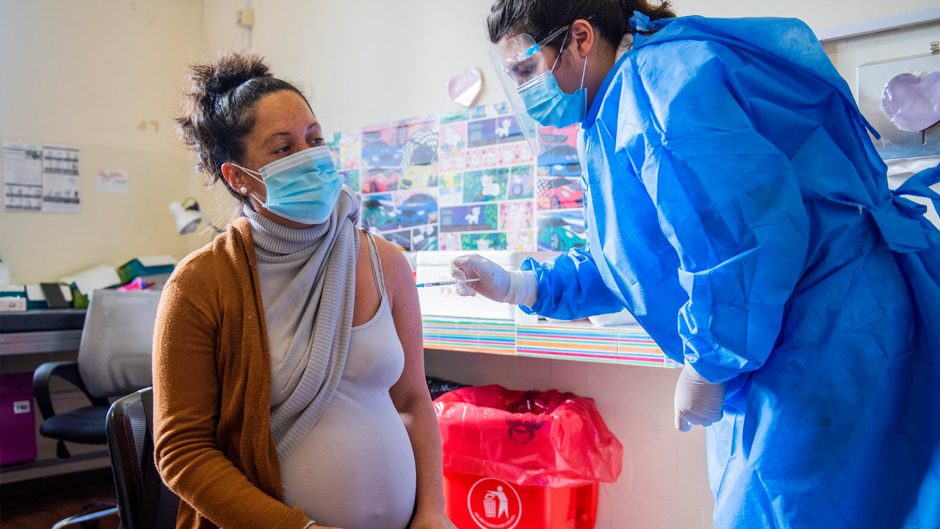
As soon as vaccines became available for COVID-19 in the United States, women who were pregnant or trying to conceive began wondering about the safety of the new vaccinations. Initially, they were directed to discuss the issue with their doctors. But today, a growing number of obstetrician gynecologists, including many from the University, are joining the American College of Obstetricians and Gynecologists, the Society for Maternal Fetal Medicine, and the U.S. Centers for Disease Control and Prevention (CDC) in recommending that women who are pregnant, or trying to conceive, get the COVID-19 vaccine.
And like the CDC, University of Miami medical experts also agree that teens should get vaccinated. Recent statistics from the American Academy of Pediatrics show that only about half of Florida adolescents who are eligible for the COVID-19 vaccine have received the injection, and nationwide about 32 percent of those between the ages of 12 to 17 are fully vaccinated, with the numbers inching up each week.
Also, while new headlines have questioned whether COVID-19 vaccines impact the menstrual cycles of teenage girls and women, University gynecologists said the possibility is unlikely.
Two physicians who study reproductive health help to clarify some of these issues for women and parents.
Michael Paidas, M.D., is an obstetrician gynecologist who serves as chair of the Department of Obstetrics, Gynecology, and Reproductive Sciences in the Miller School of Medicine. He is also service chair for UHealth Tower and the Jackson Health System, and is a clinician scientist, who takes care of patients while also conducting research on COVID-19.
Judith Simms-Cendan, M.D., is an obstetrician gynecologist as well as the division director of Pediatric and Adolescent Gynecology in the Miller School’s Department of Obstetrics, Gynecology, and Reproductive Sciences. She also serves as vice president of the North American Society of Pediatric Adolescent Gynecology.
What are the risks for pregnant women during COVID-19? And should they take extra caution before getting vaccinated against this virus?
Paidas: I have taken care of high-risk pregnant patients through what is now the fifth peak of the COVID-19 pandemic as a maternal fetal medicine physician.
Most of the patients I have treated for COVID-19 were unvaccinated, and I can tell you that getting COVID-19 while you’re pregnant is risky. Right now, with the current Delta variant, my patients are sicker, and they are more likely to go to the Intensive Care Unit. We actually had a maternal death recently that was related to COVID-19.
Overall, when you look at the national picture, there has now been about 105,645 cases of COVID-19 during pregnancy with 124 maternal deaths. So unfortunately, the risk of a mother dying is roughly 1 in 1,000 and therefore, death among mothers with COVID-19 is not uncommon. That’s about the average risk for a woman to have a blood clot in pregnancy.
COVID-19 is dangerous both in and out of pregnancy. But for women who are pregnant and contract COVID-19, there is a higher risk for pre-term birth and blood pressure problems, such as preeclampsia, especially with the more severe forms of COVID-19. And the vaccine is safe. The vaccine is not associated with miscarriage, male or female infertility, nor pregnancy complications. My overwhelming message is for women to get vaccinated (unless they are allergic to something in the vaccine).
It’s safe. So, get the vaccine as soon as you can get it. We’re in a pandemic, and it’s far more important for pregnant women to have the protection of antibodies that will last several months, than to be without them.
Is there any certain time during pregnancy that is optimal to get the COVID-19 vaccine?
Paidas: You can get the vaccine while trying to conceive, at any point in your pregnancy, and while breastfeeding. There are benefits to the vaccine besides protecting your own health. If you get it during pregnancy, the antibodies will cross the placenta, reach your baby, and afford them some protection, too.
If the mother has already had COVID-19, should she get vaccinated?
Paidas: If you’ve had COVID-19, pregnant women should still get the vaccine after they are over the acute illness stage. This will help bolster their immune response even more.
What would you tell women who are trying to conceive and are still hesitant about getting the vaccine?
Paidas: The studies so far on the vaccine are reassuring that there is absolutely no effect on male or female fertility or conception rates.
What do you think of reports in the news that COVID-19 vaccines could affect the menstrual cycles of women and adolescent girls?
Simms-Cendan: The impact of the pandemic on adolescents has been huge, and there are many statements from groups like the American Academy of Pediatrics that confirm this. Teens have suffered from isolation, poor school performance due to the challenges of virtual learning, food and housing insecurity from lost parental income, the loss of family members because of COVID-19, or fear for the health of vulnerable family members.
Adolescents often have crazy sleep patterns due to stress, lack of exercise, and excessive screen time. And one of the most common reasons that adolescent girls sometimes present with prolonged, irregular periods are because they are not ovulating yet.
Many providers during the COVID-19 pandemic have seen very irregular bleeding patterns in teens—independent of vaccination—because adolescent girls often have irregular cycles. Their brain-ovary-uterus communication system doesn’t function as well as it does in adult women and major stressors and illnesses completely throw off their cycles.
Teens receive many vaccines during puberty and adolescence and there’s no vaccine that has ever been shown to cause irregular periods.
To echo Dr. Paidas, there is no evidence of the effect of the COVID-19 vaccine on fertility or pregnancy and there is currently no evidence to show that the COVID-19 vaccines cause irregular menses. Meanwhile, the effect of the pandemic on adolescents overall is profound.
Paidas: There is now an interest in studying the COVID-19 vaccine with respect to women’s menses. That’s not to say there’s a problem, but there’s enough interest in looking at it. The menses is often called the fifth vital sign because it is sometimes seen as a measure of how a woman is doing. A lot of things affect the menstrual cycle like stress and other issues, so the question is what are those factors? And is the vaccine one of them?
So far, the evidence we have on this is only anecdotal, but the chatter has raised to the point where the National Institutes of Health is looking at this. So, that’s why there is active work about to be launched in the area.
From a biological perspective, the way that the majority of these vaccines are working, it’s not altering anything genetically. I also don’t think there’s a reason why the vaccine would be causing issues to have any immediate or long-term effect at all to the reproductive system. So, if we have an approval for it, people should be getting the vaccine. I don’t think we are going to see a negative signal about it. But the studies are being done now, so we will find out. But I would suspect it will be fine.
What about parents who are still on the fence about getting their teen vaccinated?
Simms-Cendan: There are so many reasons for adolescents to get vaccinated. Chief among them is that it will protect their health. For example, one in three people who get COVID-19 get long-haul COVID-19. That means if they get that type of COVID-19, it will pull them out of school constantly.
Also, teens don’t typically live in a vacuum. So, you are protecting the entire world around them from a possible infection—other children in the house, older adults in their family, etc. While this vaccine is new, the vaccine has been shown to be safe, while COVID-19 is not.
Originally published in News@TheU. Written by Janette Neuwahl Tannen.
Tags: COVID vaccines, covid-19 in Miami, Dr. Judith Simms-Cendan, Dr. Michael Paidas, pregnancy and covid
