Robotic or Open Surgery? A New Study Informs the Decision
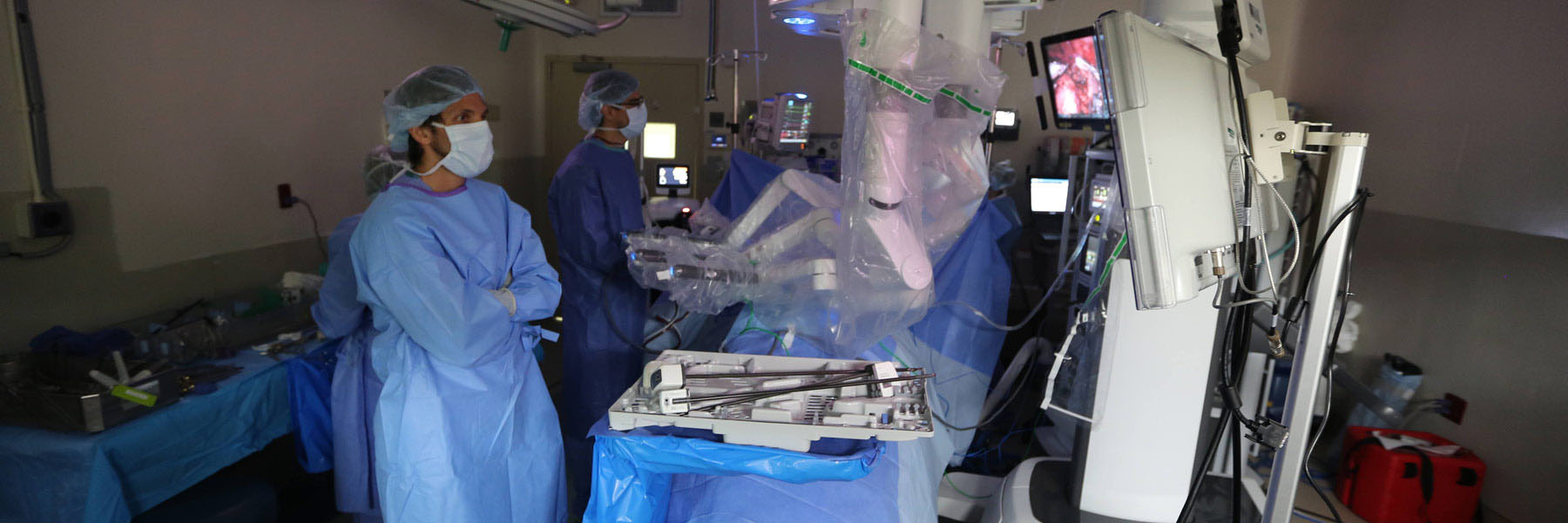
The first major study comparing patient outcomes after robotic surgery to those of traditional open surgery is published in the June 23 edition of The Lancet.
The conclusion? Robotic methods are equally effective in treating bladder cancer.
The seven-year study was conducted at 15 institutions nationally, including Sylvester Comprehensive Cancer Center. It was directed by Dr. Dipen J. Parekh, chair of urology and director of robotic surgery at the University of Miami Health System.
Known as the Randomized Open Versus Robotic Cystectomy (RAZOR) trial, the study found advantages of minimally invasive robotic surgery:
- Less blood loss
- Lower blood transfusion rates
- Shorter hospital stays
A total of 350 bladder cancer patients participated in the trial. Half of them received open surgery and half received robotic surgery. The researchers found no difference in complication rates between robotic and open surgery patients. Patient follow-ups were performed for two to three years. The two-year progression-free survival rate – the number of people who didn’t get worse – was nearly the same.
“No one had followed these patients over a period of time to find out if you are impacting their cancer outcomes with this robotic approach,” says Dr. Parekh. “We were able to prove unequivocally that we are not compromising patient outcomes by using robotic surgery.”
So, what does this mean for patients?
“Patients will also have more solid information as a result of this study and future research,” Dr. Parekh says. “The patients will ask better questions, and the physicians for the first time will be able to answer these questions, based on data rather than based on intuition. This is the highest level of data one can get.”
According to Dr. Parekh, the study demonstrates the need to conduct more trials since robotic surgery is used to treat other organs affected by cancer. “There’s a steep cost to robotic technology, and there is a learning curve, so we need to build on this in terms of making rational, data-based decisions.”
Previously, it was believed that robotic surgery patients feel they have better quality of life than patients who have open surgery. RAZOR study participants reported a significantly better quality of life after surgery, but neither group reported more advantages than the other.
Some critics of robotic surgery express concern about the lack of tactile feedback, or what you learn from touch, which is an important guide in open surgery.
“When you do robotic surgery you don’t feel anything,” Dr. Parekh says. “It’s more by visual cues. If you’re doing open surgery you have the organs in your hands, you can feel them, and you assess and do these surgeries accordingly.” The da Vinci robot used by Dr. Parekh provides a magnified, three-dimensional view of the organs, and a wide range of motion and flexibility.
Ultimately, Dr. Parekh believes that the study will guide discussions between patients and their doctors about the benefits and risks of various surgeries for complex conditions. It also shows that more high-quality trials are needed to evaluate new technologies before physicians put them into practice.
Members of the University of Miami Health System contributed to this report.
Tags: bladder cancer, Dr. Dipen J. Parekh, minimally invasive surgery, Randomized Open Versus Robotic Cystectomy, RAZOR trial, robotic surgery, Sylvester Comprehensive Cancer Center
