What is Basal Cell Carcinoma?
When the White House reported that President Joe Biden had undergone surgery for basal cell carcinoma, the announcement focused public attention on the most common type of skin cancer, one that South Florida dermatologists and oncologists see regularly.
“We see it, if not daily, certainly weekly,” says Shasa Hu, M.D., a dermatologist with the Sylvester Comprehensive Cancer Center and the University of Miami Health System. “And though it’s more common in older people, we’re also seeing more younger people developing it because of the use of tanning beds.”
According to the American Cancer Society, about 4 million cases of basal cell skin cancers (BCC) are diagnosed each year.
But Dr. Hu believes this number may be an undercount because some cases aren’t reported. This is not necessarily an intentional oversight. Rather, it’s because some cases of basal cell cancer can be treated effectively in a physician’s office without recording them in state cancer registries.
The risk of getting BCC at least once is about 39% for a Caucasian man, according to some estimates. In Caucasian women, about 25% may develop it at least once in their lives. So, it comes as no surprise to dermatologists that Biden, an older white man who is blue-eyed and fair-skinned, has developed skin cancer in different body areas.
Biden had several non-melanoma skin cancers removed as well as several pre-cancerous lesions treated before he became president, according to his private physician. What’s more, First Lady Jill Biden, who has some of the same risk factors as her husband, had three skin lesions removed in January, one of them a basal cell carcinoma.
In BCC, the skin’s basal cells — the cells under the epidermis — develop a mutation in their DNA.
The cancer is usually found in areas where the skin is exposed to the sun, such as the face, neck and lower legs, because long-term exposure to ultraviolet rays can cause cells to mutate. Of course, basal cell carcinoma can develop in parts normally protected from the sun, but these cases are not as common.
Aside from fair skin and chronic sun exposure, other factors up the risk of developing BCC: a family history of skin cancer, the use of radiation therapy to treat medical conditions, immune-suppressing drugs such as those used after transplant surgery, and arsenic, which is often found in contaminated well water or at some job sites. Certain genetic diseases can also lead to skin cancer.
The most common sign of BCC is a change in the skin. “People come to the office and say they have an area that doesn’t heal,” Dr. Hu says. “It keeps scabbing over, or the spot gets very itchy and irritated.”
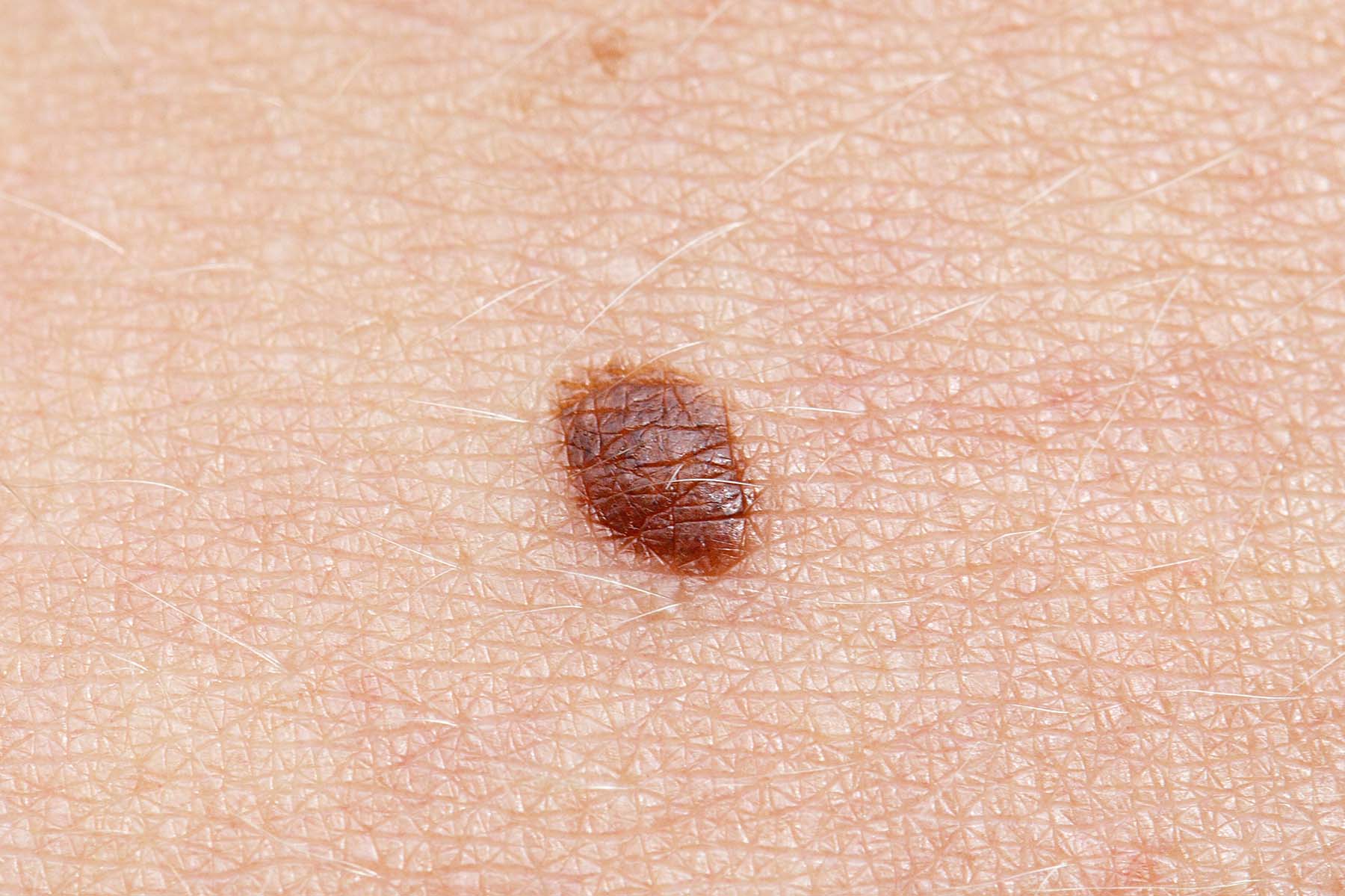
Usually, these spots are shiny and translucent, a pinkish color on white skin and brown on darker skin. It can be scaly and without a clearly defined border. In some cases, the lesion can be slightly raised as well. Over time these spots grow without treatment.
To the layman, “they can masquerade as a benign mole,” Dr. Hu says, which is why it’s important to be examined by a doctor as soon as possible.
Basal cell carcinoma, which is curable in almost every case, shares some of the same symptoms as the more serious melanoma.
(However, unlike BCC, which rarely metastasizes, melanoma can spread first into nearby lymph nodes and then to more distant parts of the body.)
“We don’t want to scare people, but we do want to encourage them to act promptly,” Dr. Hu adds. “It’s very important to get checked right away when you notice any difference [in your skin].”
The sooner the lesion is biopsied and diagnosed, the quicker an individual can undergo treatment. Depending on the location and size of your cancer, surgery is the most often used method to remove cancer and some of the healthy skin around it.
In one type of surgery known as MOHs, the doctor excises the cancer layer by layer, examining each removed strip under a microscope until no cancer cells remain. Mohs is typically used in the facial area, or when BCC has a higher risk of coming back or when the cancerous area has been radiated, Dr. Hu says.
Another treatment is called electrodesiccation. It involves scraping off the surface cancer with an instrument and then burning the base of the cancer with an electric needle.
You can cut the risk of developing BCC if you’re consistent and careful. Here are Dr. Hu’s suggestions:
- Wear sunscreen, a minimum of SPF 30, every day. Apply it on your face and any other area of exposed skin, making sure to repeat this every couple of hours.
- Avoid blistering sunburns. Dr. Hu advises parents to use extra caution with young children who are exposed to harsh UV rays in the playground or the backyard, not just the beach. One or two blistering sunburns can double a child’s lifetime risk for melanoma, the deadliest form of skin cancer.
- Wear a wide-brimmed hat and large UVA or UVB sunglasses for extra protection.
- Wear SPF-rated clothing. You can also use tightly woven garments that cover your arms and legs if these aren’t available.
- Don’t use tanning beds.
- Stay inside between 10 a.m. and 3 p.m. when the sun is most intense.
- Get skin check-ups regularly at your dermatologist. At home, you can also examine yourself for any changes to moles or bumps.
- Seek help as soon as you see an unusual spot or patch on your skin or when you notice any change to existing moles or birthmarks.

Ana Veciana-Suarez is a regular contributor to the University of Miami Health System. She is a renowned journalist and author who has worked at The Miami Herald, The Miami News, and The Palm Beach Post. Visit her website at anavecianasuarez.com or follow @AnaVeciana on Twitter.
Tags: cancer care in Miami, Dr. Shasa Hu, squamous cell carcinoma, type of cancer, type of skin cancer
