Hyperbaric Medicine Delivers Hope and Healing
Hyperbaric oxygen therapy (HBOT) is a game changer for many people.
It’s been used to help them bounce back from a diving accident, radiation injury, non-healing wounds, diabetic ulcers, surgery involving skin flaps, and many other conditions.
How HBOT works
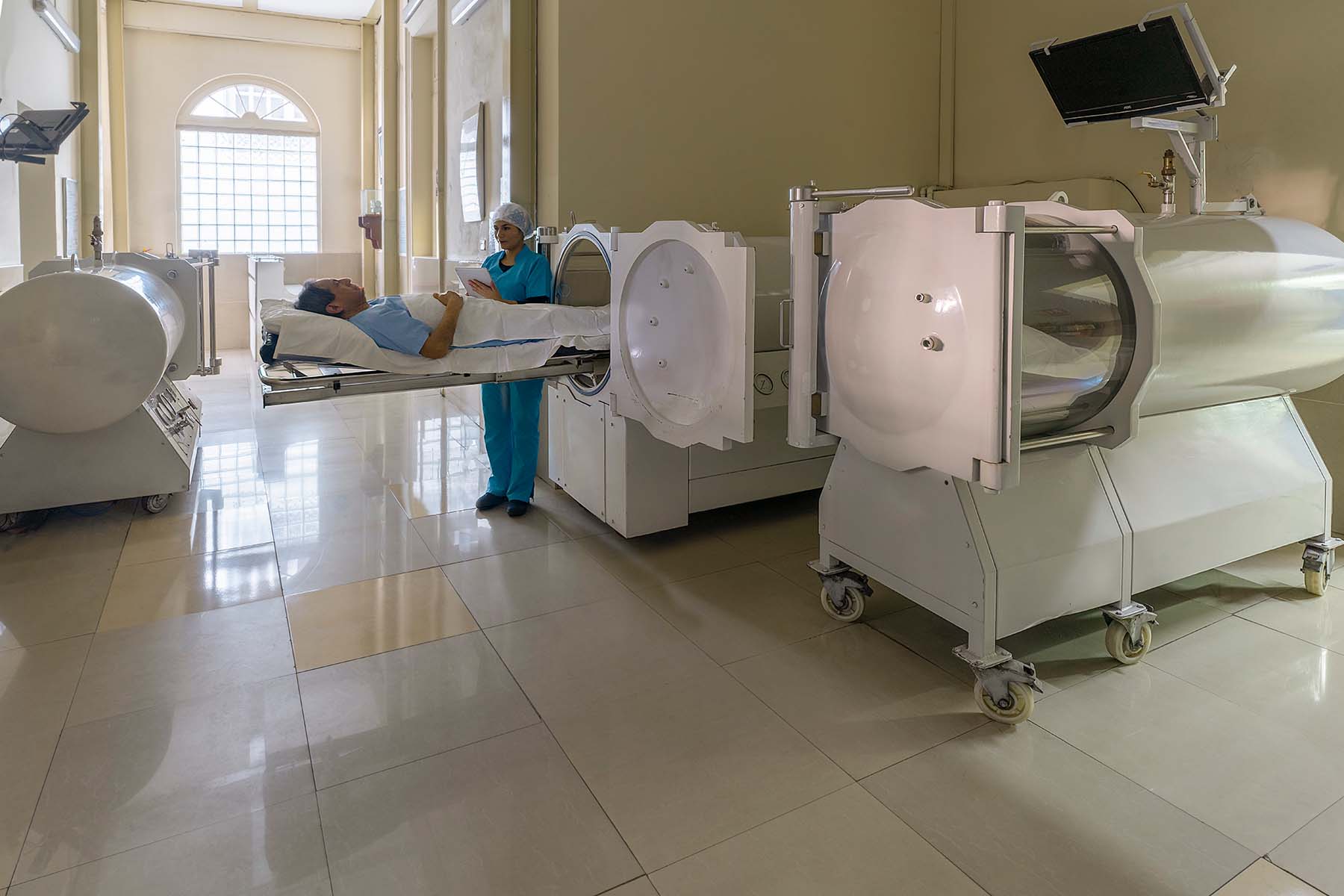
Hyperbaric therapy promotes healing by removing free radicals, optimizing blood flow, and delivering high degrees of oxygen to a wound. By increasing oxygen in the blood, HBOT allows oxygen to pass more easily through the plasma and into wounds. During therapy, the patient lies inside a clear hyperbaric chamber for about two hours.
While in the chamber, they’re surrounded by 100% oxygen at higher than normal atmospheric pressure. The process is painless and safe. In fact, many patients use their hyperbaric sessions to watch movies, rest or sleep.
According to Monica Perez, RN, more people should know about this healing method. Perez is director of the University of Miami Wound Healing & Hyperbaric Center. UHealth’s facility follows evidence-based medical practices and is the only South Florida HBOT center staffed by nurses trained in hyperbaric therapy. “Everyone else has techs, paramedics or other providers,” Perez says. “Only RNs can do a full assessment.”
Though traditionally used to treat dive patients with decompression sickness or “the bends”, Perez and her fellow team members use HBOT to treat 14 other conditions.
A therapeutic tool
“When people have a wound, we can put on all the bandages in the world, we can do a skin graft, we can provide the best technology, but if there is no blood flow in that wound, it is not going to heal,” Perez says, adding, “It’s very satisfying to know we are able to help patients heal. We are part of their journey and a tool in the toolbox.”
HBOT helps keep skin and other tissue viable after surgery, including procedures for transgender patients. We are able to help these patients when their surgeries result in non-healing wounds,” Perez says. “It’s a real game changer.”
It’s also useful for cancer patients whose soft tissue or bone tissue is damaged by radiation treatment. “Hyperbaric treatment is the only antidote to radiation injury,” says Angelina Meza-Suarez, RN, the center’s safety director.
The center assisted the construction company that built a major tunnel linking Watson Island to the Port of Miami. “Their workers used an elevator going down more than 100 feet. Even though they were not in the water, they could still get ‘the bends,’ and we took care of some workers when they brought the elevator up too fast,” Perez says.
Hyperbaric medicine was introduced at the University of Miami in 1996-1997 by Dr. Ronald Samson, a former U.S. Navy SEAL and current anesthesiologist at the University of Miami Health System.
Dr. Robert E. Marx, a dentist at UHealth, pioneered the Marx protocol, a widely accepted hyperbaric treatment for treating problems associated with radiation injury in head and neck cancer patients. Dr. Marx is one of several doctors on UHealth’s hyperbaric medicine team.
Nancy Moreland is a contributing writer for the UMiami Health News blog. She has written for several major health care systems and the Centers for Disease Control and Prevention. Her writing also appears in the Chicago Tribune.
Tags: decompression sickness, diabetic ulcers, HBOT, hyperbaric chamber, Monica Perez, radiation injury, Robert E. Marx, Ronald Samson, the bends
