Should I Have Heart Surgery in the Era of COVID-19?

By Joseph Lamelas, M.D.
Chief of Cardiac Surgery
As we restart the economy and resume our lives, there is no doubt that our new normal will look different.
This change will also happen in the workplace. For me, that is the University of Miami Health System, where I am the Chief of Cardiac Surgery.
We have implemented a new normal, with numerous protocols that allow both our patients and our healthcare personnel to remain safe and take comfort in proceeding with the care that can no longer be put off.
For the protection of everyone, we are testing all patients that are having cardiac surgery for COVID-19 prior to the date of their procedure, as well as all people involved, including our operating room team and me.
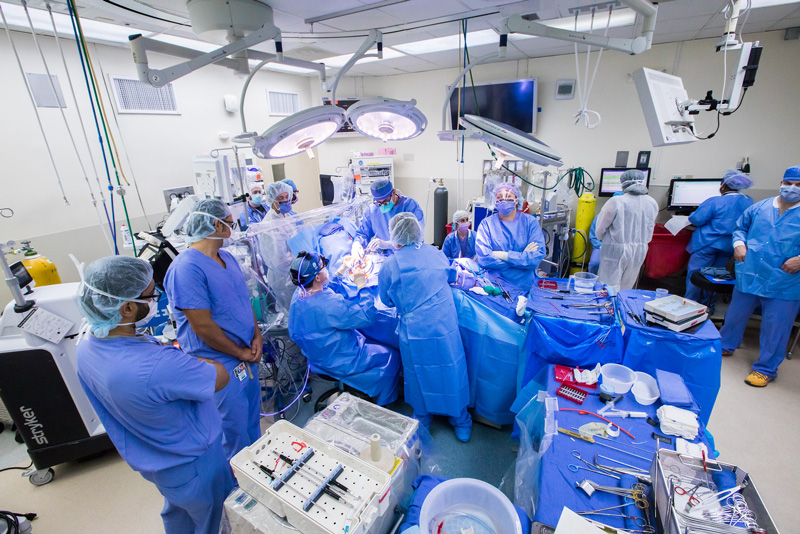
Our anesthesia team takes special precautions when intubating our patients. Our entire operating room team wears additional personal protective equipment.
This is all done in addition to testing our patients for COVID-19. A negative test is required before entering the hospital for elective surgery.
For added safety, patients admitted with COVID-19 are cared for on a completely different floor with staff and physicians that only care for them. The teams do NOT cross-cover.
We are currently not allowing our patients to be accompanied by family members, but this may change once we have the capability to add testing for family members. While this may seem frustrating, it is a necessary precaution we must take at this time in order to protect our patients and our healthcare workers who risk their lives daily to care for patients in need. The less exposure to others that we and our patients have, the safer our environment is for everyone.
A patient can also rest assured that we have implemented an impressive communication system. We keep each patient’s family informed throughout the operation, and I personally call the family after the surgery. When the patient arrives in the Cardiac Surgical ICU, the intensivist also calls the family. Later in the afternoon/evening, the ICU nurse and the cardiac nurse practitioner once again call the family where they are provided with a phone number to call the ICU. Once the patient is extubated, which is usually one to four hours after arrival to the ICU, staff can assist the patient in actually seeing their family members on their phone or other platforms. Once they are transferred to the telemetry unit, the communication continues with our telemetry staff. We take pride in becoming their new family members of our patients during their short stay in the hospital.
Time is of the essence when you have a correctable cardiac surgical disease. Your heart may not wait until the pandemic is over.
Our cardiac surgery patients’ stays are shorter because of the method of surgery we utilize for most qualifying patients, called The Miami Method. This minimally invasive, sternal-sparing approach to cardiac surgery is made through a two-inch incision on the side of the chest and results in less physical pain and trauma, less blood loss, reduced risk of infection, shorter hospital stays, quicker recuperation, and better long-term outcomes than more traditional cardiac surgical procedures. It can also be used in high-risk patients such as those who are elderly, obese, or have other comorbidities.
We have extensive experience in performing the Miami Method, having performed more than 7,000 of these types of surgeries that allow us to treat a multitude of cardiac pathologies. These include replacement of the aortic valve, repair or replacement of the mitral valve, repair or replacement of the tricuspid valve, multi-valve repair or replacement, replacement of the ascending aorta and hemi-arch, repair of congenital cardiac defects, removal of intra-cardiac tumors, arrhythmia surgery, and even coronary bypass surgery.
We have systems in place that permit us to perform multiple cardiac surgeries on a daily basis with efficiency and excellent results. This has translated into having one of the lowest morbidity and mortality rates in the country. Because of this, we have become the busiest cardiac surgical center, with one of the largest volumes of cardiac patients in Florida.
At UHealth, we have a comprehensive approach to the care of our patients and strive to improve the delivery of care every day.
Patient safety is our number one priority.
It is crucial to proceed with heart surgery once indicated. We all have fears during these unprecedented times, but developing COVID-19 in addition to existing cardiac disease will lead to poor outcomes. Time is of the essence when you have a correctable cardiac surgical disease.
Your heart may not wait until the pandemic is over.
I encourage patients and families to NOT be concerned proceeding with heart surgery, even during the pandemic, as long as hospitals prepare themselves accordingly and deliver exactly the same results and outcomes as before.
Place your heart in our hands, and we will get you through this.
